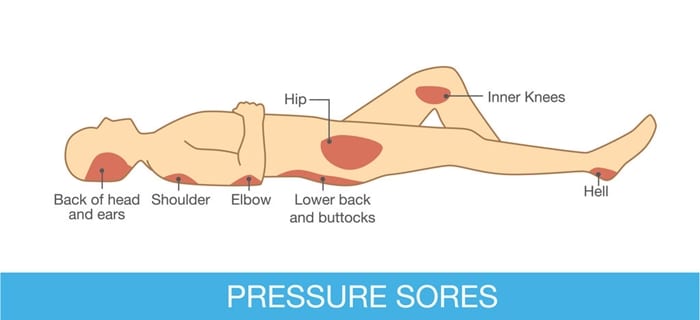
Relieve Pressure on the Skin – Rotate Pressure Areas
- Lift and turn your family member away from areas where boney areas press the skin against the bed or other hard surfaces, previously receiving all the pressure based on their sitting. When helping them move, do not slide them because sliding causes friction, which may tear the skin. If possible, try to help them change positions at least every two hours. (Think about how stiff you get if you don’t move after sitting in the same position for a long time)
- Use foam wedges or pillows doubled over and tucked under a person’s back to help gradually reposition someone onto their side.
- Pillows placed under elbows, between knees, ankles, and wrists/hands help keep the bones in those locations from rubbing together and becoming painful. Padded washcloths, cushions, and wedges may also help.
- Use pillows, wedges, washcloths, or anything soft and flexible to help you reposition. The better padded the bony areas are to keep them from rubbing, the less likely they are to develop pressure ulcers; however, don’t put so many objects in the bed that the person gets overheated, either!
- To help with sweating, you can put a little corn starch in the creases to help with the friction rubs. Corn starch is better than talcum powder because it has fewer chemical additives.
Positioning
- Use air, gel, or (4 inches) foam mattresses to relieve pressure against the patient skin. Beds that raise and lower the head or feet are also nice to help change positions.
- Smooth out wrinkles under the patient as much as possible.
- Don’t let heels or elbows lie directly against the bed. Instead, have them hang over the edge of a cushion or pillow or apply elbow or heel protectors.
- Perform a range of motion exercises to all joints regularly to prevent contractures and improve circulation to body tissues.
- Reposition in bed at least every two hours using wedges and pillows.
- Prevent bony body parts from lying directly on the bed.
- Keep the body in proper alignment.
- When sitting in a wheelchair, assist the person in shifting positions every 15 minutes.
Use Sunscreen – Protect Skin from Sun Exposure
- Many medications “May cause sensitivity to the sun” as a possible side effect. Therefore, use sunscreen, sunblock, and protective clothing when exposed to sunlight for extended periods.
- Remember sunblock on cloudy days as well or when riding in cars.
Incontinence (Accidents) – Clean Skin Thoroughly of Irritants
- If bowel or bladder accidents happen throughout the day, clean the skin with a no-rinse cleanser with a neutral pH to avoid becoming irritated from the high extremes in pH levels associated with urine feces.
- Use absorbent underpads or undergarments that wick moisture away from the skin if leakage is problematic.
- Bowel or bladder retraining problems may be useful to help with managing accidents. In addition, it may be possible to use a bowel or fecal containment or pouching system or an indwelling catheter for severe cases.
- In addition to the prolonged pressure from being in one position, excess moisture is often present in sweating or urine/stool incontinence (accidents).
- Bladder or bowel incontinence (accidents) is a significant irritant to the skin. If urine or stool stays on the surface for an extended period, it creates skin damage and begins pressure ulcer formation. Urine and stool also contaminated the wounds and led to infection.
- White vinegar is a good agent for cleaning a non-irritated skin surface to restore the pH balance and kill bacteria. In addition, it helps eliminate odor and prevents irritation from developing. I use it a lot to stop fungus from growing.
- Cover areas exposed to urine, sweat, or feces with a barrier cream containing zinc oxide, or use vaseline to coat the skin to protect it from irritation.
Bath Time
During bath time, use warm water, not hot, because hot dries out the skin.
- Use mild soaps that are pH balanced with normal skin and non-irritating (no fragrances or alcohol to dry out skin).
- Check around tubes or devices for any irritation and clean those devices thoroughly. Clean starting from the body outward so that you do not bring germs toward the body.
- Gently apply moisturizer to all skin surfaces after the bath to keep it moist but don’t massage it; gently rub it on, so you don’t damage delicate blood capillaries.
- Apply a barrier cream with zinc oxide or moisturizing ointment to the skin and a protective dressing after cleaning the area.
- Use gentle tape for applying bandages, not the type with many adhesives, and use just enough to keep it in place. Let clothing maintain the dressing when you can.
YouTube Video Resources
Pressure Ulcer Prevention: A Guide for Patients and Carers Produced by tissueviabilityservice6704
Published on Jul 2, 2015, Nottingham City Care Partnership provides specialist wound care advice and therapies for patients with healing problems. This video contains valuable guidance on how to prevent pressure ulcers.