Recognizing Skin Breakdown
When Something Doesn’t Look Right, What Does It Mean?
When the Skin Changes Color, What happens?
When skin first starts to break down, one of the first things you see is a change in skin color due to a decrease in blood flow to the area. The pink skin makes it easier to see changes occurring in light-skinned people because blood vessels lie near the skin’s surface. In darker-skinned people, skin color changes are not as easy to detect. When trying to detect changes, look in fingernail beds, lips, mucous membranes of the mouth, the arm and hand’s underside, and the whites of the eye.
Skin Color Changes
Color | What It Means | ||
| Pale, white, ashen, gray, waxy, or translucent-like skin that’s frozen into ice | Very poor blood flow | ||
| Bluish or gray (cyanosis) could almost look purple around the lips. | Skin isn’t getting enough oxygen. | ||
| Red, dark pink, like a deep blush | Carbon monoxide poisoning, high fevers, sunburn, mild thermal burns, or any time the body can’t get rid of its high heat levels | ||
| Yellow (called jaundice) | Liver disease |
What is the Significance of the Change in Body Temperature if Skin Damage Occurs?
- Normally skin temperature is warm to the touch. If it feels hot, the person likely has a fever (above 99.1oF), sunburn, or hyperthermia (dangerously high body temperature).
- Skin is cool in the early stages of shock, plus the person sweats profusely. Other conditions that cause cool or cold body temperatures include heat exhaustion, profound hypothermia (low body temperature due to cold exposure), and frostbite.
Can you Detect Any Changes in the Skin’s Moisture Levels when it breaks down?
- The skin is normally dry.
- Wet, moist, dehydrated, and hot skin is abnormal.
Does Skin Break Down affect the Capillary Refill Timing?
The capillary refill test determines the circulatory system’s ability to restore blood. Press your thumb against a fingernail bed firmly until the bed turns white. Release pressure. The nailbed should return to normal in 2 seconds. (The nailbed is the nail area closest to the finger).
Wound Drainage
While healing, wound drainage, or exudate, is common in many wounds (including open wounds). Knowing the type of wound drainage, you might experience can help determine if the wound is healing properly. Some normal wound drainage looks like thin, watery fluid, whereas others may resemble clear blood fluid. Some types of drainage from wounds indicate infection and the presence of bacteria, while others are perfectly normal.
Infected Wound Drainage
You usually see pus, fever, swelling, and pain with infection. Pus is a thick, yellowish-white, or green liquid made of dead white blood cells, bacteria, and tissue debris and often has a foul odor and may be thin to a thick consistency. If there is blood in the drainage from an infected wound, it may leak fluid with a cream-coffee appearance. The skin around the wound may be warm to the touch. The wound may appear red and inflamed. If you see red streaks branch out from the wound, that’s a sign that the infection may be spreading to your bloodstream. Infection in your blood is severe. Contact the doctor immediately to report this development.
Types of Wound Drainage
Knowing the common drainage types is important if you need to care for a wound. The drainage color can help you know if the wound is healing properly or if wound drainage indicates signs of infection.
- Serosanguineous. Thin watery drainage that has a pink to darker red color.
- Sanguineous. Dark red drainage (usually blood) appears from deep wounds.
- Serous. Thin watery, clear fluid often drains from wounds as they heal.
- Seropurulent. Thin watery drainage is serious but has a milky, coffee-cream color, indicating an infection in the wound.
- Purulent. Milky white drainage oozing from wounds usually indicates infection.
- Hemorrhagic. Dark red blood drains from the wound and may come out in spurts due to arterial damage or the wound not healing properly.
Skin Breakdown Causes
Prolonged Pressure
Prolonged, unrelieved pressure to one area, frequently seen around a bony area such as the tailbone, hips, heels, ankles, or elbows, often causes the skin to break down.
Decreased Blood Flow
The constant pressure causes damage by decreasing the blood flow to the skin and traumatizing the area. As the traumatized area rubs against the surface it touches (sheets, wheelchair cushions, etc.), the friction starts tearing away surface cells, and tissue is damaged. Other contributing factors, such as moisture from fecal or urinary incontinence, poor nutrition or hydration, and generally poor health, often interfere.
Recognizing Skin Breakdown
Inflammation
Inflammation is usually the first sign of pending trouble. You see redness, heat, swelling, pain, and fever-like infection with inflammation, but there is no pus. You may also see blisters, wearing away or tears of the skin in the affected area, breaks in the skin, maceration (softening or whiteness), swelling, itching, and development of a blue color to the skin.
Blanching
You want to check to see if the skin is still blanching. The skin blanching if you push on it, and it gets lighter in color and then returns to its natural color once the pressure is released. That color change indicates there is still enough blood flow to that area that tissue death is not occurring yet.
Stages of Skin Breakdown
There are Four Stages of Skin Breakdown and Pressure Ulcer Development
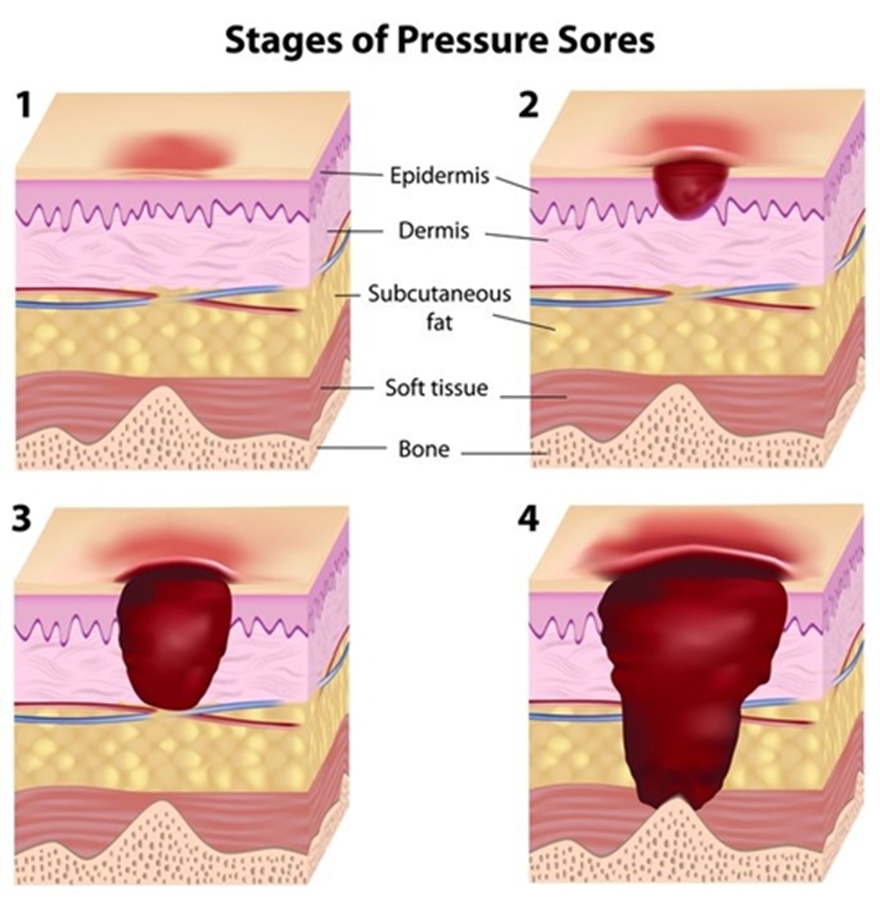
Stage I: Pre-Open Wound
An area of skin with no open sores but has changed in color, texture, or temperature is considered stage 1 of skin breakdown. The skin is still attached but appears red and discolored (greyish, ashen). It doesn’t blanch when you push on it or blanch (i.e., lighten). It may also be painful, firm, soft, warm, or cool.
Stage II: Open Wound
The pressure ulcer looks like a shallow, pinkish-red bowl-like wound or may appear to be a blister that hasn’t popped yet or has deflated.
Stage III: Deep Wound
Stage III Ulcers are deeper wounds and look like a crater, often exposing the fat layer of tissue. In addition, the bottom of the wound may have yellow deed tissue called slough present.
Stage IV: Extensive Tissue Loss
Substantial scar tissue loss has occurred by this point in time. The wound exposes bone, muscle, and tendons. In addition, the bottom of the ulcer contains slough and dark, crusty dead tissue (eschar). The serious damage is extensive and takes a long time to heal.
Starting a Treatment Plan after Recognizing Skin Breakdown
Upon recognizing skin breakdown, it’s important to begin immediately to take steps to repair the damage. If you don’t, the destruction of the skin occurs. If your initial efforts are not successful, call your doctor for advice. However, before doing so, collect specific information to share.
Size/Dimensions
Get an accurate measurement of the wound.
- Place a tape measure across the middle of the wound and measure from the two greatest distances apart in a straight line. That is the length measurement. Record it in centimeters and inches.
- Do the same thing across the center from top to bottom to obtain the width measurement–distance from point A to B in a straight line. Record it in centimeters and inches.
- If much tissue appears damaged, you must know how deep it is. Take a sterile (or if you don’t have sterile, use a clean Q-tip (one that does not leave behind a lot of fibers).
- Dip it into hydrogen peroxide and gently insert it into the wound.
- Mark the deepest point of the wound’s edge on the stem of the Q-tip. Remove the Q-tip from the wound and measure the distance from the tip of the Q-tip to the mark in centimeters and inches.
Description
Describe any drainage that might be present
Color – What color is the drainage?
- The clear yellowish fluid containing a small blood serum is normal.
- Bright red is usually fresh blood leaking from a blood vessel.
- Clear watery fluid can also look yellowish or straw-like color in appearance is also normal and usually seen in blisters. Thick mustard yellow, however, is an indication of infection starting.
- Milky white, possibly mixed with light brown, yellow, or green, indicates infected material. It may also have an odor with the pus and be painful.
Amount
Usually, the amount of drainage is determined by what appears on the dressing. See below the description of drainage amounts.
- Lack of drainage – nothing on the bandage (for a new open wound, that’s not good because the wound needs moisture to heal)
- Scant drainage – no fluid on the dressing, but the wound is moist.
- Minimal drainage – fluid covers up to 25% (1/4) of the dressing.
- Moderate drainage – The dressing is wet and at least 75% covered in drainage.
- Heavy drainage – More than 75% of the dressing is wet. If that much drainage occurs, the wound may be having trouble healing.
YouTube Video Resources
Pressure Ulcers, Prevention, Assessment, and Stages 1,2,3,4 Produced by RegisteredNurseRN
Published on Mar 7, 2018, by RegisteredNurseRN. This video provides education on pressure injuries (formerly pressure ulcers), including stages, prevention, nursing interventions, and common pressure ulcer sites. Stage 1, 2, 3, and 4 pressure injuries, unstageable pressure injuries, and deep-tissue injuries receive reviews.
******************************************