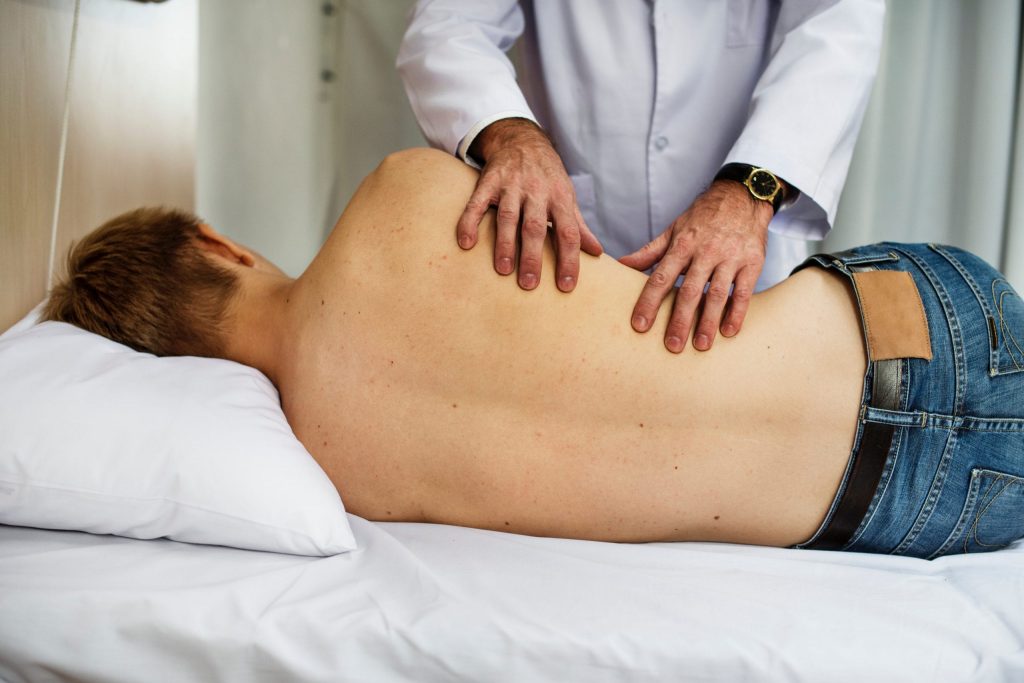
Preventing Skin Breakdown
If your family member is immobile, they are at risk of developing skin breakdown. Learn the warning signs and ways to prevent breakdowns from occurring.
Family Needs Information
Information on skincare, immobility, and fall prevention are essential bits of information for all caregivers. If caring for someone fragile, a fall can lead to broken bones and a long-term stay in bed with a downhill run toward total loss of independence within a few short months. Prevention is a caregiver’s primary defense against such an occurrence.
Once a person is completely on bed rest, if the caregiver is not familiar with skincare and how to position it to prevent skin breakdown, the development of pressure ulcers often occurs due to a lack of knowledge about how to prevent them. Once they start, they are difficult to heal. Often, the wounds become infected, and the infected wound leads to sepsis (infected blood).
Bedrest Leads to Pressure Ulcers
Falls and skin breakdown both are disasters leading to the early death of family members all too often. Before the early death, for weeks and months of pain and discomfort for both the caregiver and family member. If you learn to do good skincare and wound prevention early and know how to safely do a transfer, you can likely prevent this from happening. Lynn has been immobile for over ten years and has only had quarter-sized skin breakdowns a few times. It can happen, but you must be diligent and take it seriously.
Preventing Skin Breakdown Must Be Priority
Preventing skin breakdown must be a priority for anyone who is mobility challenged. Having a pressure ulcer can “put you on the bench” for months and change your life forever. The fact is that anyone with limited mobility, general weakness, a condition that affects their circulation, or decreased sensory perception is at risk for developing a pressure ulcer. Even someone who has recently had surgery or received sedation can develop a pressure ulcer if left unattended in the same position for an extended period. Therefore, checking daily for signs of pressure ulcer development is essential for early detection and treatment. Preventing skin breakdown before a problem develops is the best treatment for pressure ulcers.
Lack of Circulation Makes Skin Breakdown Common
Unfortunately, skin breakdown is common due to a lack of circulation to tissue when someone is limited in their movements. What is easy to develop is difficult to cure. I’ve seen a small dime-size wound develop into a ¼ inch recessed wound with drainage in a week. It can double in size within another week if it becomes infected and not treated. Infected wounds can cause permanent damage to nerves and bone leading to amputations. Those are horror stories, but they do occur. Complications from heart disease and diabetes, or kidney disease sometimes make healing more difficult. Therefore, preventing skin breakdown is essential because skin repair may not occur once a pressure ulcer starts.
Staying hydrated and eating a nutritious meal is fundamental to preventing skin breakdown. In addition, healthy skin has a greater ability to stretch and resist tearing.
Drink Water
- Drink plenty of water and other non-caffeinated liquids frequently. If you wait until you are thirsty, you are already becoming dehydrated. To stay hydrated, you need about 16 cups (8 oz) of fluid for men and 12 cups for women. It can be any liquid, not just water. About 20% of your fluid intake per day comes from the food you eat, leaving 14 cups of fluid for men and 10 for women.
- Use lotions with moisturizers if your skin becomes scaly or ashen due to dryness. Re-apply it as often as necessary to keep your skin moist. If you use a lot of hand sanitizer, apply it after sanitizing your hands.
- Wear gloves when using chemical products or needing to keep your hands in water for extended periods.
- Avoid using soaps that contain perfumes or other drying ingredients.
- Use a skin barrier to protect the skin from moisture or other irritants such as waste or sweat.
Eat a Well-Balanced Diet
- A poor diet intake (deficient in meats and water) and poor health contribute to bedsores’ formation.
- Eat protein every day. Protein builds cells and replaces tissue when it becomes damaged. Protein consists of black beans, eggs, cottage cheese, oats, turkey breast, quinoa, fish, pistachios, Greek yogurt, hemp, chia and flaxseeds, almonds, and lentils.
- Add fat, fiber, and carbohydrates to round out your calories. Eat various foods to balance vitamins and minerals, and then you won’t need supplements.
- However, if you have difficulty getting a balanced diet, try consulting a dietician regarding adding supplements to your diet to help with tissue repair.
- Drink water throughout the day to keep the skin moist.