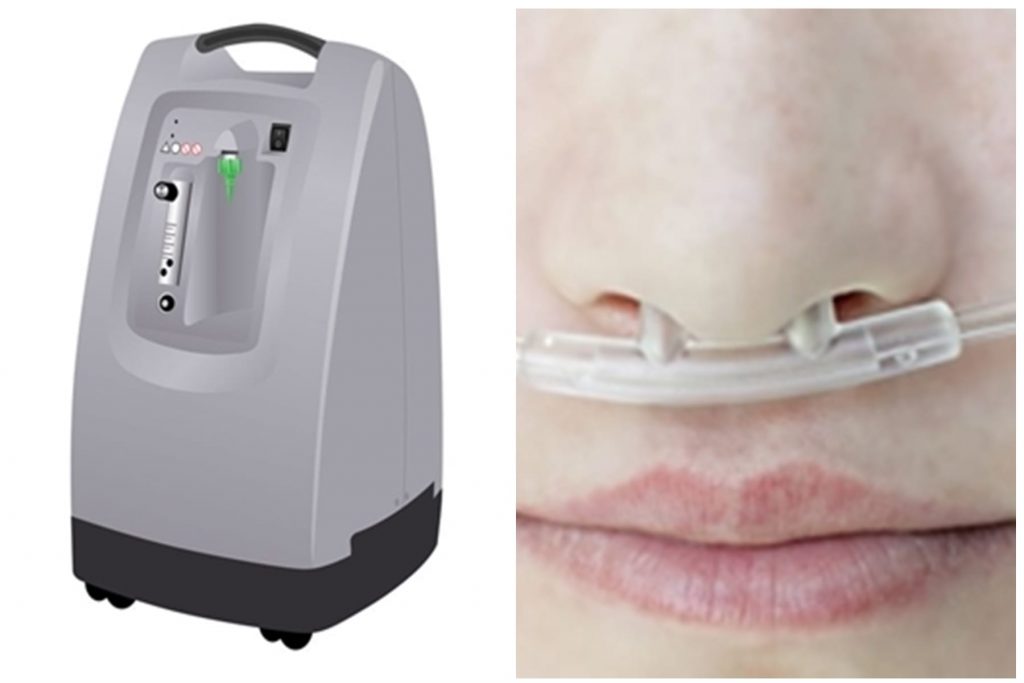
Oxygen Therapy
It may surprise you to know that oxygen is a regulated drug. Like all other medications, it has a therapeutic dose, known side effects, and risks associated with misuse; therefore, using it requires a doctor’s prescription. Although you can buy small bottles of oxygen in pharmacies to support climbers or runners, and anyone can purchase an oxygen concentrator over the internet, if you want to use oxygen as therapy and have insurance pay for it, you must do it under a doctor’s care.
Truthfully, using oxygen incorrectly can be dangerous. If a person with emphysema receives high oxygen doses, they could lose their trigger to breathe. Unlike most people, emphysema patients respond to high concentrations of carbon dioxide (CO2) as their trigger to take a breath rather than low levels of oxygen; if they receive high doses of oxygen, CO2 levels decrease, causing them to lose their trigger to breathe. Someone who did not realize that fact might see them struggling to breathe and increase their oxygen therapy, thinking they needed more to help them breathe better. Instead, they become sicker.
Why Supplement Oxygen is Needed
The need for supplemental oxygen occurs due to malfunctioning lungs or organs.
- The problem could be closed-off air sacs due to atelectasis (complete or partial).
- An over-abundance of secretions clogging up air passages resulting in the need for suctioning, postural drainage, or drugs to decrease secretion formation.
- Weak chest muscles can’t pull the diaphragm back and forth enough to give the lungs sufficient room to breathe in and out and, therefore, can’t complete gas exchange?
- Fluid backing up into the lungs due to a malfunctioning heart pump resulting in congestive heart failure.
- The kidneys stop eliminating water, resulting in extra fluid filling the lungs, making breathing difficult.
- The heart becomes fragile and can’t circulate blood preventing oxygen from getting to the lungs.
In each of these situations, the individual’s minimum requirements for acceptable oxygen levels require supplemental oxygen. The amount of oxygen and method of delivery depends again on why the person cannot get oxygen in the first place.
Reference:
https://www.healthline.com/health/oxygen-therapy
Two Types of Home Oxygen Therapy
Nasal Cannula
A plastic cannula (prongs) delivers oxygen through the nasal opening of the nose.
Advantage: safe and simple to use; comfortable, allows movement, eating, talking, and can be adjusted to any shape or size face.
Disadvantage: Can’t deliver oxygen concentrations above 40%, may cause headaches, dries out mucous membranes if the flow rate is above 6 L/min, comes out of the nose easily.
How to Use: Hook the cannula tubing behind the ears and under the chin. Slide the adjuster upward under the chin to secure the tubing. If using an elastic strap, position it over the ears and around the back of the head. Don’t apply it too tightly. Provide humidification at a flow rate higher than 4 L/minute. They can be washed with liquid soap and rinsed with water once or twice a week to keep them clean. Replace nasal cannulas every 2-4 weeks. If you get a cold, replace them once your symptoms are over.
Simple Mask
Oxygen flows through an entry port at the bottom of the mask and exits through large holes on the mask’s side.
Advantage: Can deliver concentrations of 35%-50%
Disadvantages: Hot and confining, may irritate the skin, tight seal required, may cause discomfort, interferes with talking and eating.
How to Use: Place the mask over the nose, mouth, and chin and mold the flexible metal edge to the nose’s bridge; adjust the elastic band around the head to hold the mask firmly but comfortably over the cheeks, chin, and bridge of the nose. If you can’t get an air-type seal, try taping gauze over the check area to help make a seal. The mask’s flow rate must be at least 5 L/min to flush expired CO2 from the mask to prevent rebreathing. Replace the mask every 2-4 weeks. If you get a cold or flu, change the mask when your symptoms are gone. Keep the mask clean by washing it with soap and water and rinsing it thoroughly.
Reference: https://medlineplus.gov/ency/patientinstructions/000048.htm
Home Oxygen Delivery System
Oxygen Tanks
Home oxygen therapy usually consists of one or two compressed oxygen tanks for travel or, in case the electricity goes out, an oxygen concentrator, tubing, and the delivery system chosen. An oxygen concentrator is a machine that removes nitrogen from room air, increasing the oxygen concentration of the room air to more than 90%. It’s less expensive, refilling is not required, and safer to use than an oxygen tank.
Clean the air filter at least twice a week and wipe down the unit with a damp cloth daily to keep it clean. However, it is loud, and it needs to have ventilation to keep it from over-heating.
Use Caution with Pressurized Tank
Take precautions with the backup oxygen tanks. They are pressurized gas. The tank could act as a missile and cause much damage if one develops a leak. Store containers in a secure stand, never in your car’s trunk or under your bed (unless good air circulation exists).
Note: The oxygen in the compressed air tanks can become combustible if allowed to come too close to a fire, and the tank is leaking — post warning signs related to combustion and possible burning.
Reference:
https://www.webmd.com/lung/lung-home-oxygen-therapy
https://copd.net/living/dos-donts-supplemental-oxygen/
Oxygen Safety
Follow these safety tips if you use oxygen in your home.
- You should post “NO SMOKING” signs on all entrances.
- When wearing oxygen, stay at least five feet away from any open flame (i.e., candles, gas stove, fireplace, campfire, sparklers, etc.)
- Don’t use flammable products like aerosol sprays, paint thinners, rubbing alcohol, etc.,
- Oxygen may make your lips, mouth, or nose dry. Use Aloe Vera or a water-based lubricant such as K-Y Jelly. Do Not use oil-based products like petroleum jelly (Vaseline).
- If your ears get sore from the tubing, ask your oxygen equipment provider if they have foam cushions to protect your ears from the tubing.
- Do NOT change your oxygen’s L/minute (flow rate) without discussing it with your doctor first.
- Take good care of your teeth and gums. The drying effect of the oxygen may make you prone to dental irritation.
- If you plan to travel on public transportation, talk to the transportation company about your use of oxygen and the accommodations needed in advance. Contact airlines in advance when flying if you need oxygen on a trip. Many have special rules in effect about oxygen.
Reference: https://medlineplus.gov/ency/patientinstructions/000048.htm