Normal Respiratory Function
To recognize when something isn’t working right, you need to know what it looks like when working perfectly. Therefore, let’s do a lesson on normal respiratory function. Don’t worry; it won’t be painful.
Overview of the Normal Respiratory Function
The purpose of the normal respiratory function is to breathe oxygen from the atmosphere and supply it to the body’s organs—the oxygen and carbon dioxide (a waste gas in the lung) exchange places during the breathing process. The gas waste product is then eliminated from the body into the atmosphere completing the breathing cycle.
The Respiratory System Has Two Tracts
The entire respiratory system has two tracts—an upper and a lower. Together they perform the normal respiratory function or exchange oxygen and carbon dioxide between the body and the air.
Upper Respiratory Tract
The Upper Respiratory Tract consists of the space in the head behind the Nose. Starting with the Nasal Cavity located directly behind the Nose, normal respiratory functions begin with breathing air through the Nose into the body. The Nose has little; tiny hairs called Cilia trap dirt and other debris to keep them out of the lungs.
Air temperatures can range from extremely hot to below zero; therefore, our bodies need something to safeguard us from the air we breathe—that’s the purpose of the Sinuses. The Sinuses are air spaces located around your Nose and in front of the skull and forehead that help regulate air temperate as you breathe. (Isn’t God amazing to think of adding that safeguard?)
So, we breathe air in through our Nose or Mouth, the Sinuses cool or warm up the air as it enters, then the air travels down the Pharynx (throat), past the Larynx (voice box), and into the Trachea, completing the pathway of the Upper Respiratory Tract.
Lower Respiratory Tract
Once past the Larynx (voice box), air enters the remaining pathway into the lungs, following the Lower Respiratory Tract.
Entering the Lower Respiratory Tract through the Trachea (windpipe) begins with a fork in the road. The Trachea looks like a tube of multiple rigid rings that fork to the left and right at the end. Due to this abrupt ending, when someone accidently inhales food, this fork creates a point where the food lodges and blocks the airway. When this type of airway obstruction occurs, the result can be minor or life-threatening food).
Using the Heimlich Maneuver often relieves the obstruction either completely or enough to allow air to keep the person alive until they can reach the hospital. All caregivers should learn the Heimlich Maneuver for such events, especially those who care for persons who have difficulty swallowing. Aspiration (inhaling food) can result in pneumonia or complete airway blockage and death. (Pardon the side-tract on risks of food aspiration)
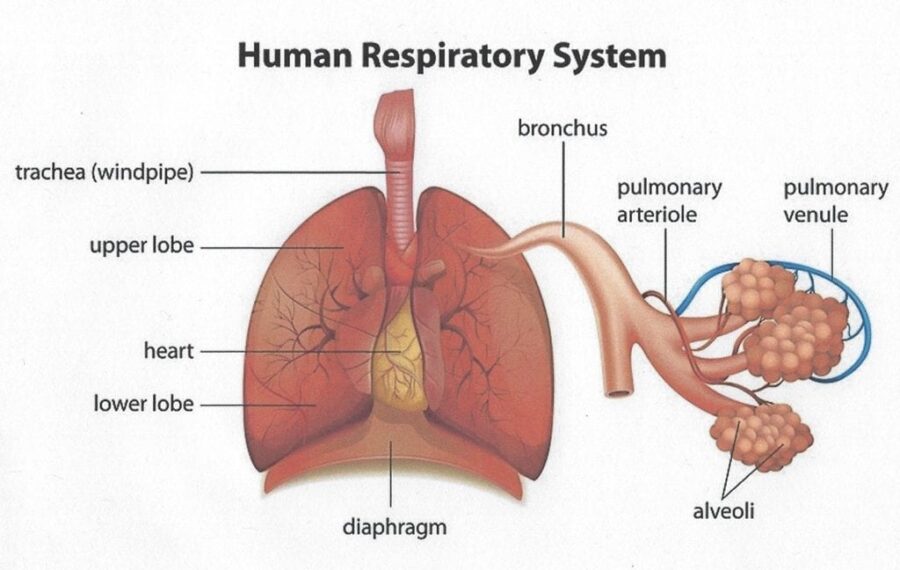
Air continues its way past the Trachea into the Bronchus Tubes (there’s one on each side of the body). The Bronchus Tubes branch out into Bronchioles that look like tree branches, with each branch of the tree ending with tiny, cloud-like air sacs (Alveoli) attached. The oxygen/carbon dioxide gas exchange occurs in the Alveoli, completing the trip through the Lower Respiratory Tract.
Gas Exchange
The oxygen and carbon dioxide (CO2) exchange happens in the smallest spaces of the lung, the Alveoli. Here’s how:
- The heart pumps the carbon dioxide-filled blood to the lungs in the veins.
- Once there, the blood releases the CO2 into the alveoli, and the alveoli exchange it for oxygen.
- The blood now leaving the lungs has become filled with oxygen and goes into the heart with fresh new oxygenated blood sent around to all the organs.
Normal Respirations
When someone is breathing normally, the chest moves up and down in a rhythmic pattern. Therefore, inhaling and exhaling take equal time with relaxation between movements.
Age | Normal Resp. Rate | ||
12 years + | 12-20 breaths/min | ||
5-12 years | 20-25 breaths/min | ||
2-5 years | 25-30 breaths/min | ||
1-2 years | 25-30 breaths/min | ||
<1 year | 30-40 breaths/min | ||
1-30 days | 30-60 breaths/min | ||
premature | 40-90 breaths/min |
Reference: Weber, Janet. (1993) Nurses’ Handbook of Health Assessment. (2nd. Ed.) Philadelphia: J.B. Lippincott Company. 142.
Lungs Sounds (Normal) Produced by RegisteredNurseRN
********************************
Normal Respiratory Function vs. Abnormal Breath Sounds – Hear the Difference
If you want to hear the difference between normal and abnormal breath sounds, the YouTube video above provides a good example of normal breath sounds.
After listening to “normal,” listen to the examples of abnormal breath sounds found on “Abnormal Breath Sounds.” In each case, the breathing is noisy and sounds stressed.
Call your doctor if your family member struggles to get a deep breath and has an oxygen saturation reading that stays below 90 or bluish tented lips. Describe what you hear. Don’t worry about putting a name to it; the doctor will do that later. Instead, focus on telling them if the sound is soft or loud, sounds wet or dry, junky, full of rattles, crackles, or other sounds described in the videos.
When Do You Treat It Yourself or Call the Doctor?
You can’t always know for sure, but most of the time, you’ll know by instinct when to call the doctor and when to treat it yourself because you know your family member. First, however, it never hurts to know the following essential pieces of information.
- Know what normal looks like for your person.
- Know your person’s usual pulse, respiratory sounds and behaviors, blood pressure, and what works and doesn’t work for them.
- Please talk with your doctor about when they want you to call, what they want you to try first, or when they prefer you go straight to the emergency room.
Respiratory Function Facts to Know
- Total Lung Capacity TC)– Gas volume for an average adult after maximum inspiration (breathing in) is 6-8 liters. The inspiration is called Total Lung Capacity (TLC). TLS increases in patients with chronic obstructive pulmonary disease (COPD) and decreases in conditions like fibrosis and restrictive disorders.
- Residual Volume (RV) – Even after breathing out all you can breathe, some air is left in the lung to keep the lung from collapsing. This left-over air is called residual volume (RV) and is usually around 2-2.5 liters.
- Vital Capacity (VC) – For most healthy adults, the typical amount breathed in and out (inspired and exhaled) is called vital capacity (VC), and that is around 4-6 liters. This amount of VC is decreased in restrictive and obstructive lung diseases because trapped air occurs in both situations.
- Functional Residual Capacity (FRC) – After a normal expiration, the lung’s volume (not when they ask you to breathe out as much as you can; just a normal breath) is called functional residual capacity (FRC). That amount is usually 3-4 liters. It increased in obstructive conditions and decreased in restricted conditions, probably due to poor muscle tone.
Resources:
********************
********************