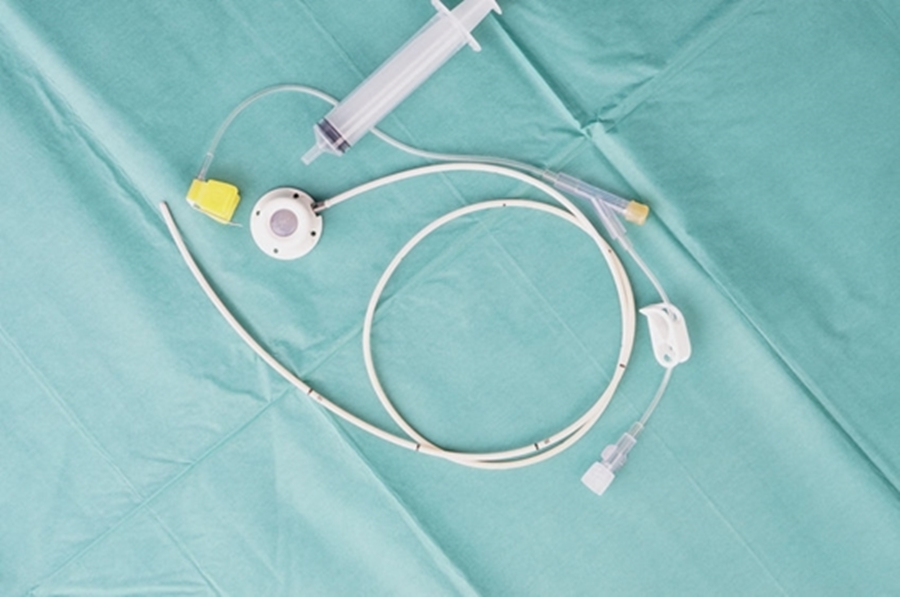
Managing Venous Catheters
Managing Venous Catheters at Home
Caregivers frequently receive responsibility for managing venous catheters (IVs) at home a few days before patient discharge from the hospital. Whether the catheter enters the bloodstream from outside the body or internally using a long catheter that ends close to the heart, family caregivers receive training in the hospital and go home to care for alone.
Usually, a nurse shows them what to do, lets them do it a few times, and once home, they have materials sent home with them from the hospital to use as reference in case anything goes wrong. Home health usually comes by the day of or the day after discharge to check on them, but their visit only lasts about an hour at most; the rest of the time, they do all the care themselves.
Most people do not realize that the procedure these family members do at home is one of the most strictly controlled procedures performed in the hospital for infection and safety precautions. It’s very risky. Not doing it correctly places the patient at risk of acquiring a blood infection. Blood infections mean any organ of the body can also become infected.
Furthermore, failure to properly secure the clamp on the tubing could allow air to enter the tube leading to an air embolus (clot), resulting in a stroke or death or allowing massive blood loss from the line through hemorrhage. As you can see, knowing what to do and how to do it safely is critical to the person’s life with the central line. Therefore, adequate training and access to quick and knowledgeable resources during emergencies are essential.
Many Types of Central Line Devices
Multiple types of central line devices exist. For example, central line catheters access the major blood vessels inside the body and are the riskiest. Though there are many types, common features exist among them.
- Using a sterile technique is mandatory every time.
- Unintentionally letting anything enter the central line can threaten the family member’s life.
- You must constantly pay attention to your every move. If you accidentally allow bacteria to get into the central line, it goes directly to the heart.
Review “5 Steps to Washing Your Hands”
Knowing how to wash your hands correctly is the #1 defense against fighting infection. I encourage you to review handwashing techniques even if you know it all. 5 Steps to Washing Your Hands is an excellent resource for reviewing germ-free work areas and sterile techniques.
5 Steps to Washing Your Hands Produced by HealthwiseOrg
Venous Catheters When Providing Home IV Therapy
Occasionally a family member receives short-term IV therapy during home. Managing home venous catheter IV therapy is much the same as home central line care. Here’s an example to show you how from YouTube.
How to Administer Home IV Fluids produced by Pruitt Health
Wash your hands using liquid soap, humming the Happy Birthday song twice
- Put on non-sterile gloves
- Remove air bubbles from all syringes by pushing the plunger upwards.
- Return caps to the end of syringes. Set aside
- Pull the plug from the IV bag. Insert the spike into the IV bag till the IV starts to flow through the tubing.
- Clamp the tubing. Hang the bag.
- Fill the chamber of the tubing about 1/3-1/2.
- Slowing open the clamp to allow removal air from the rest of the tubing. Re-clamp when all air bubbles are removed.
- Remove the cap from the end of the PIC line and set it aside. Scrub the end 10 sec. with an alcohol wipe.
- Apply Saline flush Syringe, unclamp the tubing, and inject saline using the push/stop technique until all saline is infused.
- Remove the syringe and re-apply the green cap to an IV line; if anything is touched, clean it with alcohol first.
- Attach tubing and dial-a flow rate device.
- Undo the clamp; confirm it’s dripping and that everything is working.
- Monitor Infusion till complete.
- Disconnect IV tubing from the PIC line,
- Scrub the IV line and attach the saline syringe to the flush line.
- Flush with saline using the push/stop method.
- Inject Heparin
- Clamp, Re-cap, Cover.
How to Find A Vein Produced by RegisteredNurseRN
Note: Most Caregivers do NOT start their IVs. However, knowing how to perform the technique may help prepare your family member for the procedure.
- Apply a tourniquet
- Keep the limb dangling lower than the heart
- Apply light heat, wrap the area in a blanket
- Stay away from lumpy areas (those are valves that block the needle’s progress)
- For veins that roll, tighten the fist or skin area before inserting the needle to anchor the vein.
- Angle the needle at a shallow rather than steep angle to avoid going through the vein as easily.
- When starting IVs, they must start inserting needles at the farthest point from the heart and work their way upward, or the veins above the insertion point will leak from previous missed attempts.
Steps for IV Dressing Change- No Sterile Touch Technique
Note: Caregivers usually change the IV site because that is usually done by home health; however, in some cases, it may be necessary due to the required frequency. If venous access is needed regularly, a porta cath is usually inserted instead.
- Gather necessary supplies
- Wearing sterile gloves, remove old dressing careful not to dislodge IV
- Carefully remove the stat lock (alcohol may help to remove it)
- Change gloves
- Using swabs to clean the site. Use swab to clean one side of PICC, flip the swab and clean another side; throw the swab away.
- Use another swab and clean sides around the site, again flipping the swab as different quadrants are cleaned. Always clean the innermost to outermost directions.
- Change gloves
- Apply stat lock
- Apply new clear dressing (date dressing, so you remember when you changed it)
Managing Venous Catheters with Central Access
Central Venous Catheters provide access to large veins in the body. The two primarily accessed are the subclavian and the internal jugular veins, which lead directly into the heart’s superior vena cava. While there are many advantages to using large veins, managing venous catheters carefully is very important. Central venous catheter therapy increases the risk of life-threatening complications such as:
- pneumothorax (hole in the lung),
- sepsis (whole-body infection),
- thrombus formations (blood clots), and
- vessel and adjacent organ perforation (punching hole in the blood vessel or organ nearby).
Therefore, if you manage a venous catheter (central line) at home, extreme care must be used whenever you access or handle the catheter. Any contamination of the line could have life-threatening consequences. A strict sterile technique is required to prevent bloodstream infections.
Central Venous Line Care Instructions
Lab Work
The following are key points to keep in mind related to lab work.
- If you have lab work ordered and someone unfamiliar is about to draw labs, remind them not to draw blood from the same line used for giving medication if two lines are available.
- Draw only the smallest amount of discarded blood allowed to keep all access limited to only essential draws.
- Try to group lab tests so one stick can get blood for multiple tests.
- Flush the site well after lab draws to decrease the risk of blood clots and possible blockage.
Flushing and Locking a Catheter
Blood has a natural tendency to clot. So if any build-up gets on the inside of the catheter, blood will begin to stick to it, and the opening will close off. To prevent that, using a heparin flush solution after each use helps prevent clots from forming.
The general rule is that when the catheter is not in use, a weekly flush is customary. During times the catheter is in use, follow this procedure:
- Check the catheter to make sure the line is open by pulling back and checking for blood flow before use each time,
- Use saline flush between doses of medications or injections of anything else to prevent incompatibility reactions, and
- Give Heparin flush to prevent clots from forming as the last step.
Keep a Dressing Over the Entry Site into the Body
Keeping an airtight dressing over the site where the catheter enters the body is essential. The reason is to prevent germs from entering the body around the catheter at that opening. Remember, that catheter takes blood, and whatever else has touched that catheter straight into the heart. Therefore, the strictest sterile technique must be used to do dressing changes, tube changes, and anything that goes with that catheter.
See-through (transparent) semipermeable (breathable) dressings should be changed every 5-7 days and gauze dressings every two days. If you see signs of infection, if the dressing comes loose, gets dirty, contaminated, or is messed up, CHANGE IT.
NEVER Remove the Catheter Yourself. Don’t. Never pull that catheter out. Only nurse practitioners or doctors can remove them. If you feel it must come out, go to the emergency room to have, a doctor pull it out. If it accidentally comes out, pressure the insertion site to prevent bleeding in transport to the hospital.
Peripherally Inserted Central Line Access – PICC Lines
A Peripherally Inserted Central Venous Catheter (or PICC for short) is a long, flexible tube that delivers fluids and/or medication into your body through a vein in your arm. Using a needle and local anesthetic, a radiologist or certified nurse inserts a thin wire to guide the catheter into a large vein leading to your heart. Once inserted, the PICC catheter allows direct delivery of medication or fluids for several weeks without using a needle or IV each time.
Managing venous catheter care after placement includes ensuring the catheter works correctly and the dressings remain dry and clean. For example, PICC catheters require a flush of saline or other fluids at least once a week so that lines do not get clogged, preventing blood flow through them.
PICC (Peripherally Inserted Central Venous Catheter (PICC) Produced by UHN Patient Education
Flushing the Central Line
- Assemble your supplies
- Wash your hands
- Open supplies for access while you have on sterile gloves
- Remove air bubbles from saline and heparin
- Put on your sterile gloves
- Scrub the hub of the central line for 15 seconds
- Clamp line and attach saline flush.
- Unclamp the line and flush.
- Clamp the line, remove syringe, and scrub the hub with alcohol again for 15 seconds.
- Attach the heparin syringe, unclamp the line and inject heparin.
- Remove the heparin syringe, and recap the end of the line.
If you want to see an example of a Central Line being flushed and the cap being changed, see the Boston Children’s Hospital Video below.
Instructions for Changing Caps on a Central Line (produced by CancerQuest ):
- Caps are changed every seven days.
- Masks must be worn during line cap changes since the line is completely open.
- The cap is primed with saline prior to being applied to the line.
- Attach the cap to the syringe by twisting clockwise.
- Before changing the clamp, clamp the line.
- Remove the old cap by twisting it off counterclockwise.
- Scrub the end of the line with alcohol for 15 seconds.
- Take off the blue end of the primed cap, insert the new cap into the line, and twist it into the line to tighten it.
- Remove the syringe.
- Unclamp the line.
PICC Complications produced by Jens Gundermann
The most common complications for PICC lines include the following:
Catheter migration symptoms (i.e., the catheter moved out of place):
Change in catheter function, change in external length of the catheter, chest pain, difficulty breathing, and irregular heart rates
Catheter Becomes Clogged or Blocked (Occluded line):
Inability to flush the line or give medication through it. Medicines won’t flow through the line or they are running very slow.
Phlebitis (inflammation) of the Vein:
Tenderness, redness, heat, or swelling at the site where the line enters the blood vessel or anywhere along the length of the blood vessel.
Infection at the Infusion Site:
Redness, swelling, heat, hardness, pain, or drainage at the insertion site. May also have a fever or a fast heart rate.
Air Embolism (i.e., an air clot that blocks off blood flow):
Lightheadedness, anxiety, confusion, fast heart rate, low blood pressure, sharp chest pain, and severe difficulty breathing.
PICC Dressing Change produced by Nurse Minder
**********************
Accessing Implanted Port Produced by Care Pro HS
A porta cath is another type of implanted central line access device often used for chemotherapy patients or those who frequently receive IV fluids. It’s a small round hub implanted under the skin and accessed by a needle. This YouTube video shows how it’s accessed and flushed.
Locate Port and gather supplies
- Prime syringes so that fluids to be injected are at the tip of each.
- For the Saline syringe, attach a positive pressure cap to the tip of the syringe.
- Push enough saline through the filter to fully prime the pressure cap.
- Open extension tubing and while it’s still in the package, attach the Huber needle (if not already attached).
- Attach all of it to the end of the filter.
- Flush the tubing keeping the syringe/filter/tubing all together in the package.
- Put on your mask and sterile gloves
- Scrub porta cath site for 30 seconds with alcohol. Let air dry for 60 seconds.
- Retrieve extension tubing with attached Huber needle on end.
- Locate the port, and hold it firmly while inserting a needle into the center of the port until the needle hits the back of the reservoir. Aspirate to determine placement.
- Flush the port with 10 ml saline using the push/pause method.
- Give medication next if ordered.
- The complete process with Heparin.
- Put transparent dressing over the needle site. Label with date.
Boston Children’s Hospital
Boston Children’s Hospital has a Home Parenteral Nutrition Educational Video Program available online for anyone to watch who is receiving home TPN (Total Parental Nutrition). While it is not a substitute for one-on-one training, it is an excellent reinforcement to training previously received or it can serve as a reminder of what to do if training was weeks ago and a cap change is needed now. Below are the titles of the videos that are available and the link to their site. Each title is connected to their page for your convenience.
Cleaning Your Hands
****************************************************
Making a Clean Work Space
*****************************************************
Putting on a Mask
******************************************************
Putting on Sterile Gloves
******************************************************
How to Flush a Catheter
******************************************************
Priming and Connecting IV Tubing
*******************************************************
Changing the Needleless Connector
*******************************************************
Changing the Dressing
*******************************************************