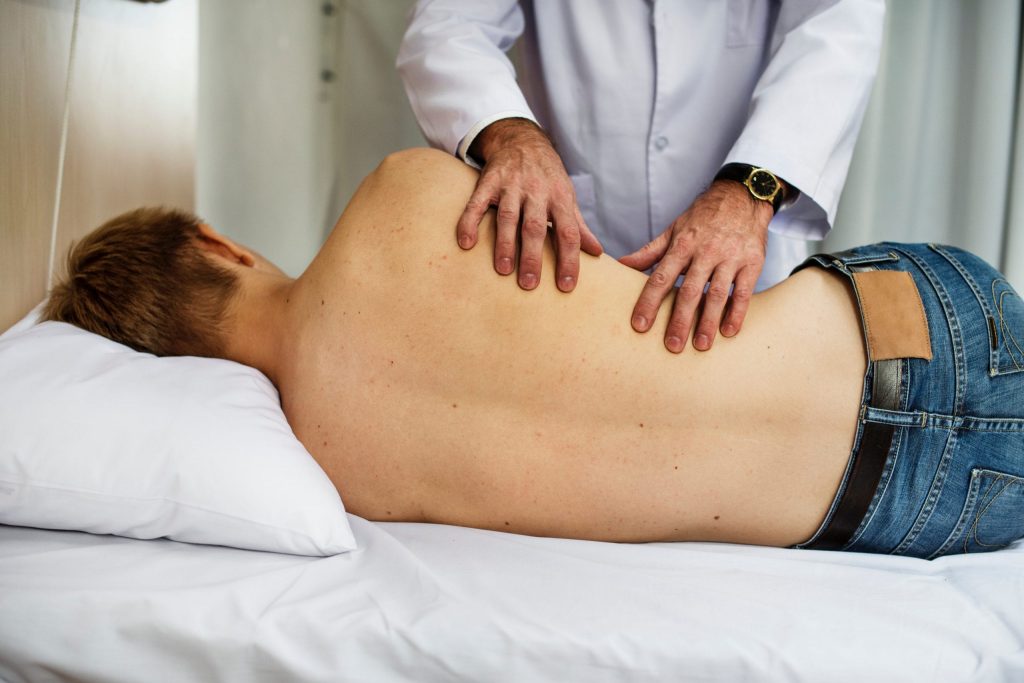
Breathing Therapy
When someone is struggling to breathe, the diagnosis’s name may help the doctor determine the course of treatment, but for the caregiver, all you want to do is help them breathe easier. Therefore, it is often useful to become familiar with both the common and unusual symptoms of a condition and the “home remedies” others have found helpful. Knowing what to expect in advance and how you might handle those issues can save you a lot of panic. Learning how to do breathing therapy at home and having the tools available in advance may save your family member’s life if time is critical.
Early Intervention Can Promote Healthier Living
Many early interventions promote healthier living or improvement in symptoms that do not require a doctor’s order. Then, as the family member’s condition changes, the doctor adds new treatments. Some of these, you will do, and some, home health do. In any case, the goal is to help your family member breathe better.
There is much you can do at home to help. For example, you have access to assistive devices, chest physical therapy, breathing exercises, and coughing exercises –all of which can provide effective breathing therapy to someone whose breathing is not normal. Provided below are examples of what you can do and how to do them.
Breathing Therapy Exercises
Diaphragmatic Breathing
With your family member sitting up straight, place your hand against their abdomen between their ribs. Have them take in a deep breath through their nose and exhale slowly. Do this focused, controlled breathing exercise about ten times per hour.
Resisted Breathing
Help your family member to sit up. Place one of your hands on each side of their chest just under their armpits (mid-way). Tell your family member to breathe in as if they are trying to push your hands off their chest. While they breathe in trying to expand their chest and internal lung space, you should gently add resistance to keep the lung from expanding.
Yawn (Inspiratory Hold)
Ask your family member to take a deep breath and hold it for 3-5 seconds. Exhale slowly. Often the exhale will cause a cough.
Chin-to-Chest Breathing
Your family member may sit, lie on their side, or sit at a 90° angle with their chin resting against their chest. First, you would place your hand against the back of their head to help them keep their head down and in position. Then, have them take a deep breath through their nose and slowly exhale through pursed lips. This exercise helps slow breathing for fast respiratory rates.
Pursed Lip Breathing
As your family member is breathing out through pursed lips (pursed lips resemble puckered lips), place your hand over the upper stomach (the V area between the ribs). As your family member breaths out through pursed lips, they contract their stomach muscles. You then start to push upward and into the diaphragm. This process helps to remove trapped air from the lungs.
Coughing Exercises Used in Breathing Therapy
Cascade Cough
Instruct the person to take a deep breath, then cough several times until they feel there is no air left in their lungs. This maneuver helps to move secretions from smaller airways to larger ones where it’s easier to cough.
Huff Cough
This technique is like creating an internal vibration feeling. First, have the person take a deep breath and do a series of “huffs” as they exhale with their mouth open. After they “huff” several times, they should try to cough.
End-Expiratory Cough
Take a deep breath, exhale slowly, and try to cough when the lungs are almost empty. It may not produce sputum, but it helps to move it from areas of smaller airways to larger ones.
Assistive Devices Used as Breathing Therapy
Incentive Spirometer
The purpose of this device is to improve lung volume. Sit up straight, seal your lips around the mouthpiece, take a slow, deep breath and blow into the mouthpiece. Your goal is to see how high you can make the ball rise and how long you can make it stay that high. Repeat this process five times, trying to make the ball go higher each time. On the fifth time, try to cough instead of blowing to see how high the ball goes.
Acapella Breathing Device
The Acapella Breathing Device is used to help remove mucus from the airways. You place it between your lips and blow through the mouthpiece. As you blow, it causes a vibration that loosens secretions, helping you cough the stuff out. It has a dial to adjust the difficulty required to create the vibration, making it an effective exercise.
Nebulizer
A medication delivery device that produces a fine mist to inhale into the lungs. The medication is carried into the lungs on the mist and absorbed through the lining of the alveoli.
Inhaler
An inhaler is a medical device used to administer medication into the body via the lungs in an aerosolized format.
External Ventilator
My husband used an external ventilator for several months. During that time, Lynn had significant difficulty keeping his carbon dioxide level from getting too high due to weak diaphragm muscles and pneumonia-related airway obstruction. He could not push the “bad air” out of his lungs because his diaphragm muscles were weak. The device saved his life by applying external pressure against his chest wall. It pushed the air down, assisting his diaphragm in doing its job. Over time, he strengthened his core chest muscles enough that he no longer needed the external ventilator, and we returned it to the company.
Chest Physical Therapy
Postural Drainage
Postural drainage aims to drain the lung of congestion using gravity. The elevated position allows the lung secretions to drain out of the smaller areas of the lung into the larger areas. Once in the larger areas, the secretions are easier to remove with coughing.
Using pillows or wedges, raise or lower the chest and arms into the desired position. Hold the position (if tolerated) for 5-20 minutes repeating the process every four hours to keep the lungs drained. Percussion and vibration work well in association with postural drainage.
Percussion
Percussion is often employed when an individual has a lot of thick, hard-to-expel secretions, as with rales (coarse crackles). To perform percussion, form your hand into a cup shape, then strike the person’s back with the open-cupped hand using a rapid, rhythmic movement.
Do NOT do this if the person has broken bones, a fresh heart attack or surgery, fragile skin, bleeding disorders, a blood clot, or a bruised lung. It is always a good idea to discuss using percussion with a doctor first before you try it the first time to be on the safe side.
Vibration
Vibration frequently follows percussion; however, use as an independent treatment is also effective. The motion used with vibration is subtle, like a quiver, not harsh like shaking. You place your hands above the lung area to receive the vibration with your arms straight; elbows unlocked. As the person exhales, you create a quiver motion with your hands, a slight tremulous motion (not a shake). Repeat the motion three times for each lung section.